| . |  |
. |
UPI Correspondent Washington (UPI) Jul 05, 2007 Hospital-acquired infections increase mortality rates and healthcare costs, and a growing number each year withstand traditional treatment. Methicillin-resistant staphylococcus aureus, or MRSA, represents the most dangerous form of staph infections because it can't be cured by normal antibiotics. The percentage of MRSA infections has steadily increased since the 1980s, and a recent study conducted by the Association for Professionals in Infection Control and Epidemiology suggests the numbers are higher than anyone suspected. The national study found 46 out of every 1,000 patients studied had MRSA infections -- eight to 11 times higher than previous estimates. Although hospital-acquired MRSA infections pose a threat to patients, an emerging and more deadly strain has begun to circulate outside of medical centers, said Richard Wenzel, president of the International Society for Infectious Disease, in an interview with United Press International. Q: How serious of a problem are MRSA infections in the United States? A: They've become very common infections ... What we're seeing today is a second kind of staph infection called community-associated MRSA, and people outside of hospitals are getting it. It's even more worrisome than hospital MRSA because the community MRSA infections almost always have a toxin called PVL (Panton-Valentine Leucocidin). When this staph gets into the lungs or blood, it's truly devastating and worse than even the healthcare-associated MRSA because the toxin chews up tissue and tends to cause shock in patients. Q: How is the disease spread in the community? A: It started in athletic teams and then in prisons. It appears to be spread through very intense sharing -- of towels, sometimes water, even soap or through touching cuts. Recently, doctors in New York found staph in the vaginal area of some patients, so it can be spread as a sexually transmitted contact disease as well. Any kind of close contact -- on people's hands or close contact with the genitalia -- can spread staph infections. You may remember a couple years ago, some of the Los Angeles Rams (football players) had cuts and were bleeding, and they all jumped into a common whirlpool and a lot of the team got infected. Q: How is community-associated MRSA affecting hospital infections? A: It turns out that in the last couple of years the community-acquired MRSA have begun to spread into hospitals. At this point, it's a worry, but in the future it could become a real a problem. We'll see more patients even more ill than with healthcare-associated MRSA. It takes different types of drugs to treat the toxic-producing community strains, and it's much more difficult to get rid of it than the healthcare MRSA. It's also more difficult to identify. The hospital ones you find in the nose, but with the community one, we're not sure where it hides all the time. So we now have two epidemics: one is continuing in hospitals, but the traffic is now going two ways. To me that's the most threatening thing in the next five years. Q: Is the hospital-associated strain increasing in prevalence? A: It certainly has increased since the '70s and '80s. There were a couple epidemics then, but in the '80s, once we controlled the epidemic, only 5 percent of staph infections were methicillin-resistant, whereas today it's probably 55 percent. Q: How are staph infections spread in hospitals? A: I would say that 85 percent of the time it's on the hands of healthcare professionals. So it's patient to patient, but on the hands of healthcare workers. Q: What are the symptoms? A: It depends on the site of infection. If you have a patient who had surgery, about four days after the surgery, the area around the incision will turn red, you'll probably see puss and the patient usually gets a fever. On the other hand, if you have a patient in the critical care unit on a respirator, they can get extremely short of breath and just feel really, really horrible. Q: Is it deadly? A: If it's in a wound, most of the time a patient will survive. But if it's in the lung or the blood, I would say approximately 25 percent of patients will die within the next month. Now, these patients are also usually in a weakened condition from some other medical problem, and some die as a result of the underlying problem, not the staph infection. But at least half are directly due to the infection. Q: Some experts say treating MRSA infections in the United States has increased the cost of healthcare by extending the average hospital stay and increasing the amount of treatment needed. Do you agree? A: Any staph infection increases stay and increases mortality. The cost of that is quite significant, no question. If you have pneumonia, and you get a staph infection, you probably stay in the hospital for an extra seven or 12 days. That costs about $40,000 to $50,000. Q: What are hospitals and doctors doing to decrease the rate of hospital-acquired infections? A: Well I think the key thing is hand washing. We're doing a lot, for example, at our hospital. We have the sanitizer dispensers at each patient's bed, and that makes it easier for people to be compliant. Better use of isolation for patients who are already infected is important as well. They are put in a separate room, and anyone who enters has to put on a gown and gloves, even if they're just going to be talking with the patient. Q: What else can be done? A: I think one of the most important things that's occurred is the team-based approach to safety. We used to count on individuals to do the right thing on their own. Now we encourage staff to encourage each other to follow safety guidelines. So a nurse is empowered to say, "I noticed a break in technique, let's start over with a new catheter." Then safety becomes a part of the culture. Q: Can patients do anything to protect themselves from infections during a hospital stay? A: I tell my patients, 'before anyone touches you or any of your catheters, you tell that person "Please wash your hands in front of me and put on a new pair of gloves."'
Source: United Press International Community Email This Article Comment On This Article Related Links Epidemics on Earth - Bird Flu, HIV/AIDS, Ebola
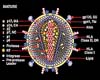 Washington (UPI) Jul 05, 2007
Washington (UPI) Jul 05, 2007Tibotec's HIV drug, TMC125, may be better at fighting resistant strains of the virus than current medications, according to two phase 3 trials released Thursday. In the trials, known as DUET-1 and DUET-2, TMC125, a non-nucleoside reverse transcriptase inhibitor, or NNRTI, suppressed virus levels better than placebo in patients who had previously been treated with other medications and had developed resistance. |
|
| The content herein, unless otherwise known to be public domain, are Copyright 1995-2007 - SpaceDaily.AFP and UPI Wire Stories are copyright Agence France-Presse and United Press International. ESA Portal Reports are copyright European Space Agency. All NASA sourced material is public domain. Additional copyrights may apply in whole or part to other bona fide parties. Advertising does not imply endorsement,agreement or approval of any opinions, statements or information provided by SpaceDaily on any Web page published or hosted by SpaceDaily. Privacy Statement |